Morton’s neuroma can be confusing and very difficult to diagnose.
Care must be taken in diagnosing Morton’s neuroma. In some cases, nerve pathology of the entire foot can be missed because the examiner mistakenly thinks that the problem is a Morton’s neuroma. For this reason, it is important to see an experienced practitioner, and they have to take a careful history followed by an in depth physical exam. Morton’s neuroma is frequently present, if it is painful to presses on the space between the third and fourth toes.
Many people will have different experiences of Morton’s neuroma pain. To some, it will feel like they are walking on a twisted bit of sock or like having a pebble in their shoes. Cramping, numbness, and burning are often reported, and the pain may radiate to other toes beyond the third and fourth ones. Some Morton’s neuroma patients feel more pain when walking over a hardwood floor barefoot.
All other diagnoses should be considered before reaching the conclusion that the pain is caused by Morton’s neuroma. You may have arthritis, a fracture, or some other condition that requires a different method of treatment. It is important to thoroughly work up the condition with imaging and diagnostic procedures to ensure that the actual cause of the pain is Morton’s neuroma.

An examination of the foot may show a reduced sensation to the area served by the nerve affected with Morton’s neuroma. The doctor may be able to reproduce the pain by squeezing the forefoot while at the same time applying pressure to the bottom (plantar) surface of the foot directly over the affected web space.
In some cases, merely feeling or pressing the plantar surface of the foot in the affected area between the toe bones can reproduce the pain. In some cases, the doctor can feel the nerve enlargement. Your foot will also show no or very little signs of redness or inflammation. Localized swelling is not common with a Morton’s neuroma and suggests another diagnosis.
Doctors may be able to demonstrate Tinel’s Sign, which is an indication of a irritated nerve. Tinel’s Sign is demonstrated if you feel a sensation of tingling of pins and needs when the nerve affected is lightly tapped.
Mulder’s Sign may also be demonstrated. This occurs when you lie on your back. Then the doctor squeezes your foot between the bones leading to the first and fifth toes while at the same time pressing the ball of the foot in the area of the Neuroma. A positive sign occurs when you feel the pain of your neuroma in the bottom (or plantar) surface of your foot. The pain you feel with the test may spread to the area the nerve serves between the toes and sometimes a click (Mulder’s click) can also be heard. The presence of a click does not indicate a positive Mulder’s Sign – the pain must be reproduced to have a positive Mulder’s sign. See this Video. You may still have a Morton’s neuroma even with a negative Tinel’s Sign or a negative Mulder’s Sign.

Since x-rays of the foot don’t show Morton’s neuroma, an MRI or ultrasound will likely be ordered but X-rays of the foot may be necessary to exclude other diagnoses.
Magnetic resonance imaging, or MRI, is one of the most sensitive tests for Morton’s neuroma, but it is not often necessary. It is very effective in determining if this condition is present. In addition, MRIs can help to determine if the pain is caused by some other foot problem, such as a ganglion cyst or cancerous neuroma of the foot. A negative MRI does not necessarily exclude a diagnosis of Morton’s neuroma.
Ultrasound examinations of Morton’s neuroma have been shown to be as effective as magnetic resonance imaging in diagnosing Morton’s neuroma. It is a relatively simple diagnostic test; however, a negative Ultrasound does not necessarily exclude a diagnosis of Morton’s neuroma.
The presence of a Morton’s neuroma as confirmed by MRI or Ultrasound does not mean that your foot pain is due to Morton’s neuroma. Studies have shown that many patients have asymptomatic (non-painful) Morton’s neuromas in their feet. Furthermore, MRI’s and ultrasounds can sometimes miss a Morton’s neuromas that is present so a negative MRI or Ultrasound does not exclude the diagnosis of Morton’s neuroma.
MRI or ultrasonography should only be used for diagnostic purposes, and even then they should be used in conjunction with a thorough history, physical examination and possibly a diagnostic local anesthetic injection. They are not a reliable indicator of conservative versus operative treatment. Morton’s neuroma is a clinical diagnosis with the prime symptom being intermittent pain usually located between the third and fourth metatarsal heads which can frequently be reproduced by direct compression between the metatarsal heads. The disappearance of pain by local anesthesia into the painful metatarsal space (a diagnostic injection) is an important and accurate tool for the diagnosis of Morton’s neuroma.
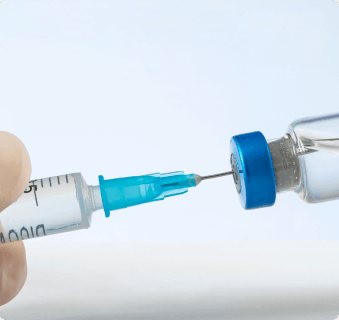
Probably the most definitive method of diagnosing Morton’s neuroma is with a diagnostic local anesthetic injection. This is considered the gold standard for diagnosing Morton’s neuroma and we do a diagnostic injection on nearly all of our patients to make or confirm the diagnosis of Morton’s neuroma.
A local anesthetic such as lidocaine is injected around the nerve in the web space between the third and fourth toes. We use ultrasound guidance to increase the accuracy of the injection and the diagnosis. If the pain is eliminated by the local anesthetic injection blocking this nerve, then a diagnosis of Morton’s neuroma is highly likely. However, if the block fails to relieve the pain, then it is more likely that the pain is caused by a different condition.
A diagnostic injection is often considered the gold standard for diagnosis. It is often more definitive than other tests and can indicate the likelihood of success of our ultrasound guided ablation procedures.
Differential Diagnosis method for Morton’s Neuroma are listed below:
The most common condition that is often mistaken for Morton’s neuroma is metatarsophalangeal (MTP) joint synovitis. This is an inflammation of the joint that connects the bones of the foot to the bones of the toes. It is differentiated from Morton’s neuroma because it causes swelling around the joint area, pain in the joint itself, and pain when the toes are forced into flexion. Your doctor can often feel the swelling of the joint by pinching the foot at the juncture at the third web space and causing pain. This reaction does not usually occur with Morton’s neuroma.
Bursitis, which is a collection of fluid in the bursa sacs that surround the joint and can present with similar symptoms to Morton’s neuroma. These bursa sacs can often squeeze the nerve that runs between the toe bones causing pain similar to Morton’s neuroma. Frequently, bursa are seen wrapped around a Morton’s neuroma and in such cases Cryosurgery will treat the bursa as well as the neuroma.
Another possible reason for pain in this area is a stress fracture of the bones of the foot or toes. This will often cause pain when the area is touched, and will show as a fracture on a simple x-ray.Pain is often felt when the affected bone is gently squeezed. Rheumatoid Arthritis and other joint problems can also cause pain in this area. They cause inflammation of the membranes around the joint that connects the foot to the toes, and it can elicit pain in this spot. Often, other joints will be painful as well, and it will not be localized to the third web space.
Tarsal Tunnel Syndrome can present similarly to Morton’s neuroma. The Tibial nerve, which is one of the main nerves of the foot, can become compressed as it passes through an anatomical tunnel in the inside ankle. In such cases the pain experienced can be similar to Morton’s neuroma. A simple clinical test called the Tinel’s test can be used to evaluate for tarsal tunnel syndrome. The test involves tapping the Tibial nerve below the ankle, and a positive test produces tingling in the forefoot. See this video
Rarely pain similar to Morton’s neuroma can be caused by an impingement of one of the nerves in the back. This is call a radiculopathy, where the problem is at or near the root of the nerve in the spine but the pain is often felt further away at the other end of the nerve. A nerve root that is constantly squeezed in the lower back (lumbar-sacral) spine can sometimes cause symptoms in the foot. Often when radiculopathy is present a simple test known as a straight leg raise will reproduce the symptoms in the foot.
A hammertoe, or an abnormal inward curving of the toe, can sometimes cause pain in the web space similar to Morton’s neuroma pain. Usually, the toe deformity is visible to the naked eye, and it can be diagnosed without further testing. In addition, pain in the area where the foot connects to the toes can be caused by arthritis of the metatarsal head joints. This is generally diagnosed once Morton’s neuroma is ruled out via diagnostic procedures, such as ultrasound-guided injection or an MRI.
Less common diagnoses that overlap with the symptoms of Morton’s neuroma include true cancerous tumors. In this case, the nerve cells may proliferate into a malignancy, but this is a rare presentation of a true neuroma. Necrosis of the metatarsal bone, such as can be present with diabetic foot ulcers, can also cause this type of pain.
Finally, ganglion cysts can form in the third web space, and these are benign, fluid filled lumps that present over the tendons or joints of the hands or feet.
We offer a number of procedures to treat Morton’s neuroma without surgery. To see the treatments we offer for Morton’s neuroma click here.

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.