What is the best way to diagnose Morton’s neuroma? Is Morton’s neuroma a clinical diagnosis? do I need an MRI for Morton’s neuroma?
Morton neuroma, a fairly common musculoskeletal condition is usually diagnosed clinically by an experienced clinician after a full clinical assessment which involves a history and competent clinical examination. However, even in the hands of an experienced clinician, Morton’s neuroma can be a difficult diagnosis to make.
The clinical symptoms are usually suggestive of Morton neuroma are(1):
Clinical signs that points to Morton neuroma are:
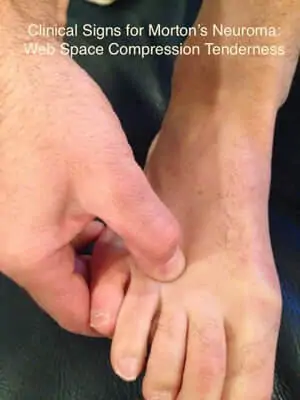
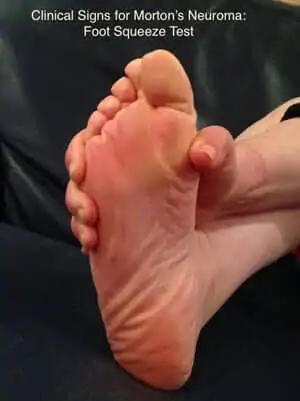
Mulder’s Sign: This test is positive in 98% patients and is usually performed with patient in the lying position. The examiner squeezes the forefoot with one hand while press the ball of the foot with other to produce characteristic pain and often a click (also known as Mulder’s click). See this Video.
Tinel’s Sign: If the involved space is pressed or squeezed, patient experiences tingling and numbness; which is a sign of nerve inflammation or involvement.
A proper history and thorough clinical examination can help in the identification of most cases of Morton neuroma; but in some cases, it is important to opt for radiological tests to help. These selective situations are:
The diagnosis can remain ambiguous after decent history-taking and examination. This could be due to a number of reasons:
The gold standard for diagnosing Morton’s neuroma is a diagnostic local injection.
Most importantly, Morton’s neuroma is a clinical diagnosis made by a clinical who is experienced in seeing and treating Morton’s neuroma patients. The diagnosis is made a after a careful assessment of the history and physical examination. In some cases a diagnostic injection may be required. It is not a diagnosis made by any radiological test whether that be an MRI or ultrasound.
References:

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.