Interdigital neuromas (also referred to as Morton neuromas) are fairly common in general population and can significantly change the lives of affected individuals if not treated correctly. See below for the 3 circumstances when a ultrasound guided diagnostic local anesthetic injection should be done.
We perform a diagnostic injection frequently to make or confirm the diagnosis of Morton’s neuroma. It is one of the most definitive methods of diagnosing Morton’s neuroma and is generally considered the gold standard.
We start by doing a careful (and gentle) physical examination of your feet to identify the one area of maximal tenderness. We then identify the nerve under ultrasound guidance and further confirm the nerve precisely with use of a nerve stimulator. Once we have confirmed the exact location, we inject the nerve with a very small amount of local anesthetic (such as lidocaine) which numbs the nerve and blocks the nerve from sending pain signals. If after numbing that nerve your Morton’s neuroma pain goes away, then we have clearly demonstrated that that particular nerve is the cause of your pain.
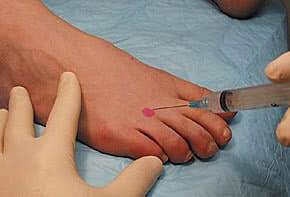
Merely seeing a Morton’s neuroma on ultrasound or MRI doesn’t actually confirm that your pain is due to the nerve since about 1/3 of the population has asymptomatic Morton’s neuroma. Feeling the maximal area of pain, identifying the nerve via ultrasound and nerve stimulator and then numbing the nerve which stops your pain clearly demonstrates that the nerve we identified is the actual cause of your pain. In other words, diagnostic local injection is indeed the gold-standard test for Morton’s neuroma diagnosis.
This diagnostic procedure is helpful in the following cases:
It has been observed that physical examination and history alone can diagnose most cases of Morton Neuroma. However, in some cases, when the symptoms overlap and physical examination is inconclusive; your physician may advise diagnostic local injection before initiating the treatment for Morton neuroma. Other situations where an ultrasound guided diagnostic local injection is used to confirm the diagnosis of Morton’s neuroma are:
The diagnosis of Morton neuroma is tricky and often times a co-existing foot pathology is missed because the examiner relies solely on the physical examination. If the pain (and other symptoms) do not respond to neve block, the diagnosis of Morton neuroma is typically excluded and other tests are needed to ascertain the cause of your pain.
Approximately 10% of all Morton neuroma cases are managed by surgical intervention after the failure of conservative treatment options. The most popular surgical intervention is a complete excision of part of the nerve and internal transfer of nerve tissue. In most cases, surgical intervention alleviates the symptoms, but in about 30% of cases, the patient may develop significant discomfort and pain after surgery.
Post surgical pain can be due to a number of causes: Stump neuroma, Biomechanical issues, a new neuroma, Post incisional nerve entrapment of dorsal cutaneous nerves, Painful plantar (bottom of the foot) scar and thinning of the plantar metatarsal fat pad. A diagnostic injection can be very helpful in resolving the actual cause of your pain.
Diagnostic local injection is often used as a prerequisite to ablation procedure. Radiofrequency ablation and/or cryotherapy ablation procedures or neurolytic injections are excellent treatments for Morton neuroma, especially when done under ultrasound guidance. In addition, these procedures are generally safe and effective in the long term and can be performed under local anesthetic agents.
Why is it helpful prior to an ablation procedure? A diagnostic injection is often considered the gold standard for diagnosis. It is often more definitive than other tests and can indicate the likelihood of success of our ultrasound guided ablation procedures.
The diagnostic local injection procedure is generally safe and effective. In extremely rare cases, atrophy of foot fat pad may occur if the solution is injected to foot pad. However, with the use of ultrasound guidance and if performed in the hands of an expert physician, the chances of developing such complications is negligible.
References:


By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.