Morton’s Neuroma Neurectomy Surgery is usually not recommended due to its high risk and high complication rate.
Should I have Morton’s neuroma surgery? (or why shouldn’t I have Morton’s neuroma surgery?)

In some patients Morton’s neuroma surgery is unavoidable because their Morton’s neuroma is resistant to any other means of treatment. However in the vast majority of cases surgery is avoidable. (We only consider surgery for Morton’s neuroma as a last option when all other non-surgical treatments have failed.)
When all other measures have failed to relieve pain, open surgery may be necessary to remove the neuroma (Neurectomy). It is critical that Morton’s neuroma surgery be performed by surgeons who have considerable expertise and experience in this surgery because in some cases, Morton’s neuroma neurectomy surgery can result in increased foot pain or even the return of the neuroma.
With the most common approach, your surgeon will make a small incision on the top of your foot (the “dorsal” approach) over the third web space. After dissecting through the tissue, the transverse metatarsal ligament is cut, to take pressure off the nerve and to allow the surgeon access to the neuroma. In most situations, the nerve itself with the resulting neuroma is removed (neurectomy). The incision is closed, and the patient is taken to recovery. With this approach, you can bear weight on your foot post-operatively, however it still takes 3-4 weeks to fully recover.
Other less frequent approaches include the plantar approach (the ball of the foot approach.) With the plantar approach, the surgeon has less tissue to dissect, and he is able to preserve the ligament, leading to better foot stability in the long term, but recovery is slow and you are unable to bear weight for 2 to 3 weeks until the sutures are removed. It can take 4-6 months of painful recovery to fully recover from a plantar approach Morton’s neuroma surgery.
In addition to multiple approaches to the surgery, your surgeon has a few options regarding how to treat the neuroma. One school of thought is to remove the offending ligaments, which then decompresses the nerve while keeping it intact.
Another school of thought is to remove the nerve that has been effected by the Morton’s neuroma entirely (neurectomy). With the damaged nerve tissue removed, the neuroma is less likely to occur, and the mechanical stresses on the foot are not increased. Most surgeons are proponents of this latter theory and remove the affected nerve, although some patients may require a different method.
Post-operatively, your course will depend on the surgical approach. For incisions made on the top of the foot, you can bear weight provided that you wear a hard-soled, loose fitting shoe. Other shoes can be introduced as the incision heals.
For plantar incision (through the ball of the foot), you can only bear weight on your heel to prevent the wound from opening and you cannot bear weight with this approach for at least 2 to 3 weeks. Physical therapy may be needed post surgery to help strengthen your foot and ankle muscles, especially if you have suffered from Morton’s neuroma for a long time causing some muscle weakness.
Surgical treatment of Morton’s neuroma is can be effective when performed by an experienced practitioner, but it comes at the cost of some risks and possible side effects.
A stump neuroma is significant and frequent complication of neurectomy surgery. Surgeons have tried many techniques, without much success, to prevent stump neuromas from growing. One of these techniques involves capping the cut nerve endings. Nerve capping techniques involve placing the cut nerve stump into the bone or muscle and covering it with a:
Placing the cut nerve stump into the bone or muscle is a technically demanding option, as the nerve stump must be properly placed into the bone hole or muscle without kinking.
There are many techniques for nerve capping because generally they don’t work.
Any surgical procedure brings with it the possible side effects of scarring and the risk of infection. Furthermore, diabetic patients may have a more difficult time healing the surgical wounds of this procedure.
When the neuroma is removed, the nerve that carries sensation to the toes is taken away as well, causing mild but permanent numbness in the forefoot and between the toes.
Some studies have shown that up to 35% of patients who have surgery end up with unacceptable levels of post surgical pain. Phantom nerve pain at the stump of the nerve can result in continuing pain and tingling. Patients can experience more pain post-operatively from further degeneration of the nerve. In many cases ongoing or worsening pain is a result of an incomplete severing of the nerve or misplacement of the nerve ending. The stump of the nerve becomes entrapped in the metatarsal bones which causes a painful sensation and in some cases, the return of the neuroma. In this situation, you may need a second surgery to bury the stump of the nerve in the musculature of the foot. For more information on post Morton’s neuroma surgery pain and stump neuroma pain click here.
Although surgical treatment can be quite effective, it is rarely performed because of the higher risk of complications and the effectiveness of less invasive procedures, such as ultrasound guided radio frequency ablation, cyrotherapy or injections of a neurolytic agent. However, for some patients, it is an effective pain treatment when performed by an experienced practitioner (frequently a surgeon) and when all other treatments have not provided adequate relief.
Should your Morton’s neuroma not respond to our ablation procedures, Dr. Pearl will confer with you and surgical colleagues here in the Boston area hospitals for a possible surgical option and we will co-ordinate your care to try to ensure that you receive the best possible treatment.
We can effectively treat Morton’s neuroma without surgery, (in many cases more effectively than surgery) and the recovery time from our procedures is only a couple of days.
For more information on the non surgical options we offer to treat Morton’s neuroma, CLICK HERE.
Surgery for Morton’s neuroma is often associated with complications, most commonly post surgical pain. In many cases the post surgical foot pain may be as bad or worse than before surgery. Some studies have shown that up to 35% of patients who have surgery end up with unacceptable levels of post surgical pain.
Post Morton’s neuroma surgery foot pain is much more difficult to treat than pre surgery Morton’s neuroma foot pain because the exact cause of your pain after Morton’s neuroma surgery can be difficult to determine. It can even be difficult to localize the exact position of your pain after surgery! Post Morton’s neuroma surgery pain can be due to a stump neuroma, nerve degradation, scar tissue or another post surgical complication. For more information on pain after Morton’s neuroma surgery (“post neurectomy pain”), click here.
Most first time Morton’s neuroma surgery is done through the top of the foot (the “dorsal” approach) which involves cutting through the transverse metatarsal ligament. Although this results in a shorter recovery time than operating through the bottom of the foot, it results in more post operative foot instability, with forefoot splaying and potential long term gait problems.
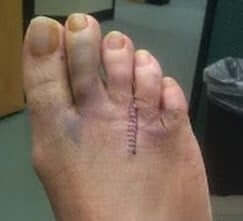
The basic recovery time from Morton’s neuroma surgery is frequently 3 or possibly 4 weeks, even if a top of the foot (“dorsal”) surgical approach is used and it can easily take 3-4 months to for the full effects of surgery. In other words, it can take 3-4 months to become fully mobile.
If another surgery is required, the success rate of a Morton’s neuroma redo surgery is considerably lower than the success rate of a first time Morton’s neuroma surgery. The redo Morton’s neuroma surgery is most commonly done through an incision in the bottom of the foot (the “plantar aspect” of the foot.) This approach results in an even longer and more painful recovery than a regular Morton’s neuroma surgery. It can take 4-6 months of painful recovery to fully recover from a redo Morton’s neuroma surgery.
There are always general surgical risks associated with any surgery and so surgery should always be avoided if possible.
However, in some cases when Morton’s neuroma is resistant to other treatments, surgery is the only option left and is unavoidable.

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.