Reviewed by Janet D. Pearl, MD, MSc
Stress fracture of the feet are minor cracks or bruising over the bone/s of the ankle or foot. Such cracks and bruising are usually a result of repetitive injuries and overuse/abuse of ankle and foot bones and are reported more frequently in athletes.
Stress fractures comprise approximately 15% of all sports related injuries(1) and affect up to 20% of all military recruits due to training-related activities. In most cases, stress fractures heal spontaneously with conservative treatment such as rest and over the counter pain medications without requiring any other medical treatment. However, putting too much pressure over a healing stress fracture can lead to delayed healing or even a complete fracture.
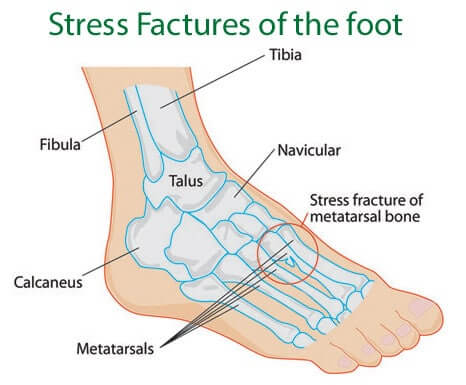
Even though the intensity and severity of symptoms may vary, the characteristic symptoms of stress fracture of ankle and foot include:

Stress fractures are caused by:
A thorough physical examination is one of the basic methods of assessing any fracture. This should start with your healthcare practitioner asking you about your medical history, drug history, activity status, occupation history etc. then a thorough examination of ankle and foot is done looking for visible or concealed signs of fracture as well as associated signs and symptoms such as tenderness and swelling etc.
Laboratory tests such as the blood levels of vitamin D and calcium are also useful to exclude metabolic factors and minimize the risk of future stress fractures.
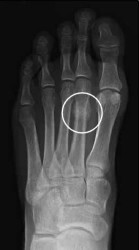
Some commonly used imaging tests to diagnose stress fractures include X-rays and magnetic resonance imaging (MRI). Both of these imaging tests are fairly sensitive and helpful in detecting stress fractures.
Treatment of stress fractures is usually conservative and non-surgical. Specific Treatments for Stress fractures include:
Rarely in complicated cases surgery may be needed. In these cases Internal fixation can done by plates, screws, and pins to hold the bones in place.
Following are preventive measures that are used for the long-term management of stress fractures:
References:

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.