Reviewed by Janet D. Pearl, MD, MSc
Morton neuroma is a common condition that is more frequent in females. According to a recent study(1), Morton neuroma is strongly linked to certain risk factors and other conditions such as intermetatarsal bursitis, chronic repetitive trauma (possibly due to wrong choice of shoes or improper gait), persistent ischemia and other nerve entrapments.

The diagnosis of Morton’s neuroma is mainly clinical. When done by an experienced clinician, a detailed history followed by thorough physical examination is sufficient to diagnose over 90% cases of Morton neuroma. That sounds simple but, in some cases, the diagnosis may be a very challenging. Here’s why:
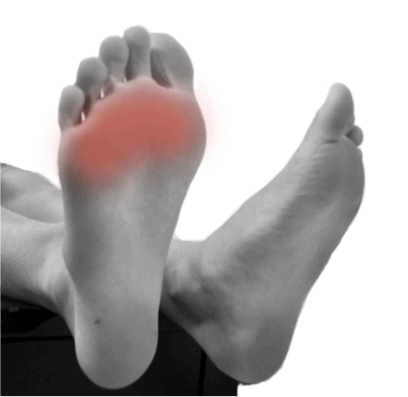
A lot of patients tend to ignore classic warning signs of Morton neuroma, especially in the early stages of neuroma formation. For example, symptoms like occasional pain in the forefoot after moderate activity or after wearing tight shoes are generally overlooked by patients as discomfort associated with activity or footwear. Most patients begin to notice Morton’s neuroma when it is advanced and symptoms are persistent or severe. In poorly managed cases, Morton neuroma can significantly alter the quality of life of an individual.
The pain of Mortons neuroma often overlaps with other foot conditions like stress fracture, tarsal tunnel syndrome, rheumatoid arthritis, ganglion cysts, hammertoe and radiculopathy etc. Many conditions can mimic Morton’s neuroma and thus make history and clinical examination challenging. For example about 5-8% of all cases of fore-foot pain that are initially diagnosed as Morton neuroma on the basis of clinical examination, are in fact due to rheumatoid nodules(2).
Foot pathologies and degenerative lesions like Morton neuroma, tarsal tunnel syndrome and other similar conditions are usually caused by chronic trauma or stress due to unhealthy gait or posture. In other words, many foot conditions share similar causes and Morton neuroma may co-exist with other lesions such as bursitis, radiculopathy, osteochondritis dissecans and rheumatoid arthritis(3). Depending upon the symptoms and severity of these other conditions, diagnosis can be complex and challenging. Failure to address an existing foot lesion can delay the process of healing and lead to other problems.
The most common site of occurrence of Mortons neuroma is 3rdintermetatarsal space; but more than 30% neuromas are reported at 1st, 2nd and 4th metatarsal spaces. Likewise, symptomatology and severity of Morton’s neuroma pain can vary from case to case, which makes it quite challenging to diagnose Morton neuroma with precision. For example, some patients explain the pain as walking on pebble; while other refers to it as a ‘dull burning ache’. Variation is also seen in the Morton’s neuroma itself. Likewise, the histopathological examination of Mortons neuroma reveal large variations(4). Degenerative changes are observed in only 59% cases. Other key features such as obstruction of blood vessels, diameter of affected nerves and rate of fibrosis also seem to differ among different patients.

Although classic clinical signs of Morton neuroma such as Mulder’s sign or Tinel’s sign are fairly sensitive in diagnosing about 60 – 80% cases; a negative result does not exclude the diagnosis of Morton neuroma(5).
The main method of diagnosis of Mortons neuroma is clinical, done by an experienced clinician, taking a thorough history and doing a careful examination. However, Morton’s neuroma can be notoriously difficult to diagnose. Many conditions can mimic Morton’s neuroma. If in doubt a diagnostic injection done under ultrasound guidance by an experienced clinician can confirm the diagnosis.
References:

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.