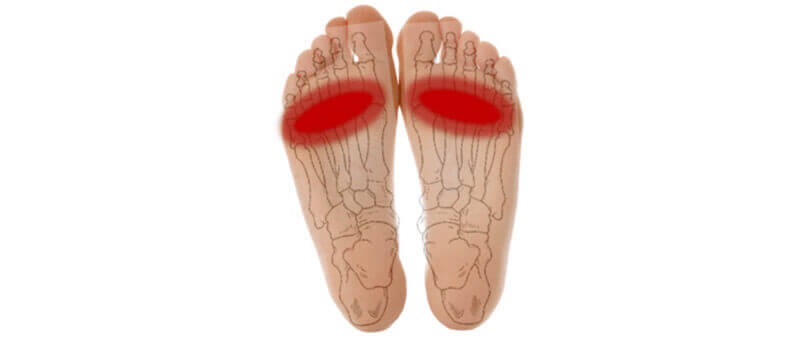
Metatarsalgia (also referred to as the stone bruise) is a leading cause of forefoot pain, especially ball of the foot pain and is frequently reported in athletes. It is characterized by inflammation of the metatarsal heads. Metatarsalgia can affect both males and females. According to some estimates, 1 of every 10 individuals develop metatarsalgia at some point in their life.

The symptoms of metatarsalgia are varied and may include:
The intensity, frequency and severity of pain in the metatarsalgia may vary from person to person.
The exact cause of metatarsalgia is not known, but it is believed that a history of strong impact of force or injury directly involving the head of first metatarsal is reported in most cases of metatarsalgia.
1. Certain triggers or risk factors(1) can influence your risk of developing metatarsalgia. Some statistically significant risk factors include:
2. Obesity and physical imbalance by causing friction-induced damage to the metatarsals.
3. Aging. The tendons and connective tissue elements change with age making a person more prone to develop this condition.
4. High arches. High arches are usually associated with metatarsal damage and recurring episodes of metatarsalgia.
5. Certain other anatomical features such as a long second toe or a hammertoe can also increase the risk of developing Metatarsalgia
6. History of gout, arthritis or other musculoskeletal conditions
The diagnosis of metatarsalgia is usually made on the history and clinical investigation/ examination by an experienced clinician. Clinical diagnosis is usually made by a combination of signs and symptoms and exclusion. You doctor should ask about your history of other musculoskeletal conditions/ ailments, your lifestyle, occupation and hobbies, and most importantly, the characteristics and associated symptoms of the pain.
The following conditions are often confused with Metatarsalgia:
Without adequate treatment the following complications are possible:
Following are some common treatments to manage metatarsalgia:
If your metatarsalgia is due to Morton’s neuroma then you should be seen by a clinician well experienced in diagnosing and treating Morton’s neuroma.
References:

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.