Morton’s neuroma, also commonly called a foot neuroma, is a clinical condition that is characterized by pain and swelling of the plantar interdigital nerve that lies within the foot. It can cause a great deal of pain and disability if left untreated, so as such needs looking into once a diagnosis is made. Medical therapy is an option with the use of orthotic devices and steroid injections being popular options, but often patients require surgery as a part of the treatment strategy. In order to perform surgery, patients will need to undergo some form of anesthesia to prevent them from having pain during the procedure.
Here we take a look at the anesthesia used when operating on a foot neuroma.
Broadly classified, there are three different kinds of anesthesia that can be used to treat foot neuromas.
1. Local anesthesia / Ankle block
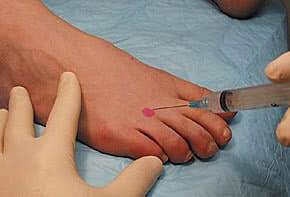
Local anesthesia refers to injection of an anesthetic agent into the skin and superficial tissues in and around the area that is about to be operated upon.
For foot neuroma surgery, local anesthesia is administered in the form of an ankle block injection where the anesthetic agent is injected directly into the ankle to anesthetize the nerve fibers that supply the foot. Sometimes, an ankle block is combined with a general anesthetic. In other cases, an ankle block may be combined with mild sedation.
2. General anesthesia
A general anesthetic agent is an agent that is administered in the form of a gas or intravenously to help patients sleep through a surgical procedure. Once the patient has been reassessed, the anesthetic agent is partly injected through the veins and the patient is asked to count backwards from 10 to 1. During this time, a mask is placed covering the mouth and nose through which a general anesthetic agent along with oxygen is passed. The general anesthesia completely knocks out the patient and prevents them from experiencing any degree of pain during surgery. General anesthesia requires more monitoring both during the surgery and during the recovery than than local anesthesia.
3. Epidural anesthesia
Epidural anesthesia is a procedure where a small needle is placed into the space between the spinal column and outer membrane of the spinal cord (the epidural space) in the lower back at the location of the nerve fibers that supply the ankle and foot.
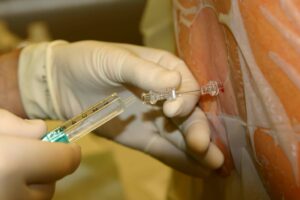
Anesthetic agent is then injected into this space and this blocks the sensation of pain from the region of the body that these nerves supply. When the procedure has concluded, the epidural needle or cannula may stay in place for a short while afterwards for additional pain relief if required.
Once the cannula is removed after the procedure, the patient is observed for a period of time to ensure that there are no side effects. Spinal anesthesia is similar except the anesthetic agent is injected directly into the spinal fluid that surrounds the spinal column and the patient has no sensation below the level at which the anesthetic has been injected.
Both spinal and epidural procedures allow for complete pain control during surgery.
Morton’s neuroma can be a painful condition that can have a negative impact on a patient’s mobility and quality of life. In order to be treated, surgical options are sometimes necessary. Performing surgery under correct anesthesia is essential. Different kinds of anesthesia are available and the choice depends upon what the surgeon feels is appropriate and what the patient prefers.

By providing us with your information you are consenting to the collection and use of your information in accordance with our Terms of Service and Privacy Policy.